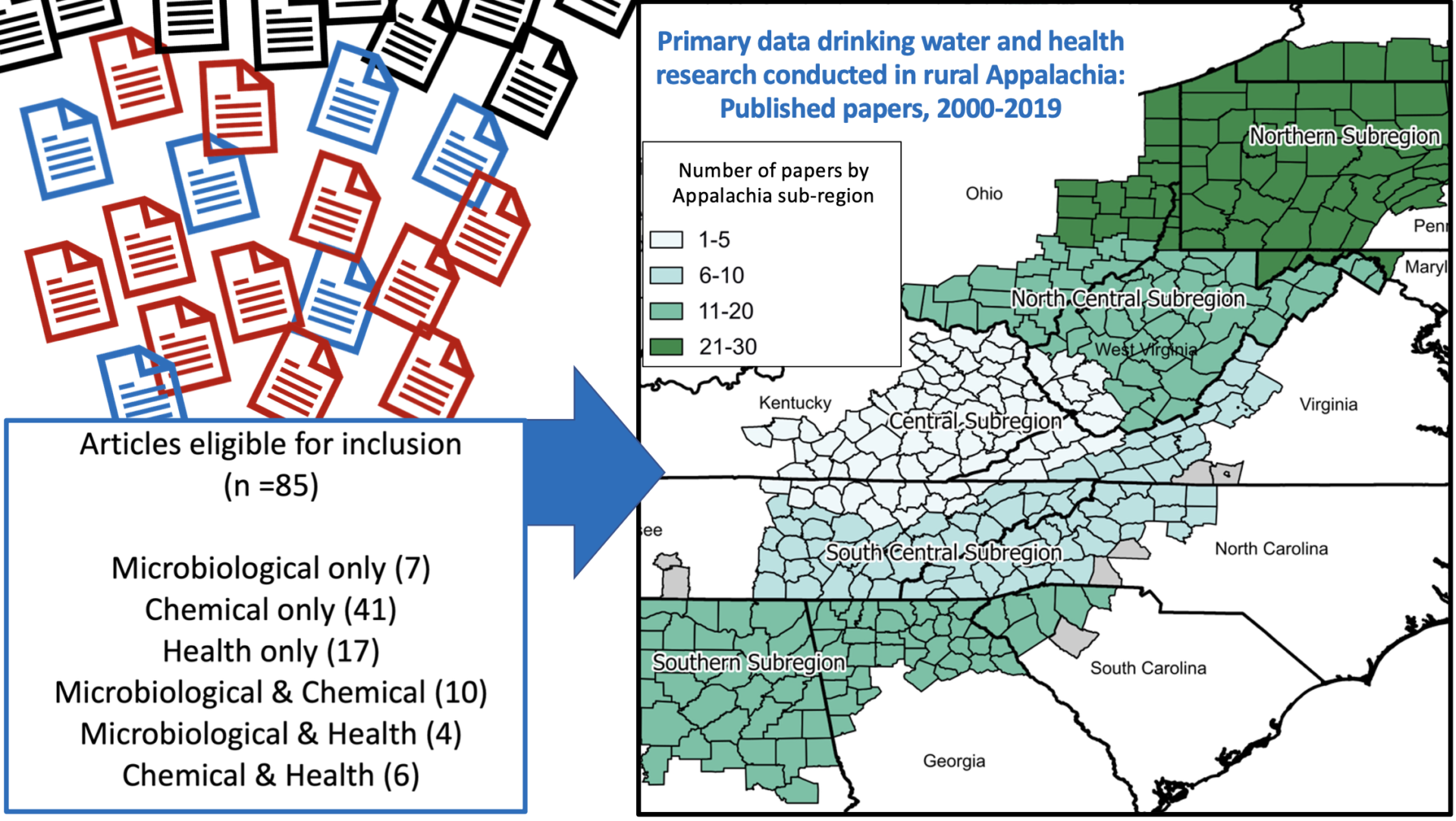
Microbiological and chemical drinking water contaminants and associated health outcomes in rural Appalachia, USA: A systematic review and meta-analysis
Authors: Darling A., Patton H., Rasheduzzaman M., Guevera R., McCray J., Krometis L.A., & Cohen, A.
Publication Year: 2023 | Journal / Publisher: Science of The Total Environment
Abstract/Summary: In rural areas of the United States, an estimated ~1.8 million people lack reliable access to safe drinking water. Considering the relative dearth of information on water contamination and health outcomes in Appalachia, we conducted a systematic review of primary data studies published from 2000-2019. Of the 3,452 records identified for screening, 85 met our eligibility criteria. Most studies were conducted in Northern (32%, n=27) and North Central (24%, n=20) Appalachia, and only 6% (n=5) in Central Appalachia. Across studies, E. coli were detected in 10.6% of samples. 32% (n=27) of studies assessed health outcomes, but only 4.7% (n=4) used case-control or cohort designs (all others were cross-sectional). The most commonly reported outcomes were detection of PFAS in blood serum (n=13), gastrointestinal illness (n=5), and cardiovascular-related outcomes (n=4). Overall, based on the number and quality of eligible studies identified, we could not reach clear conclusions about the state of water quality, or its impacts on health, in any of Appalachia’s subregions. More epidemiologic research is needed to understand contaminated water sources, exposures, and potentially associated health outcomes in Appalachia.
PDF on Publisher Website | PDF on OSF
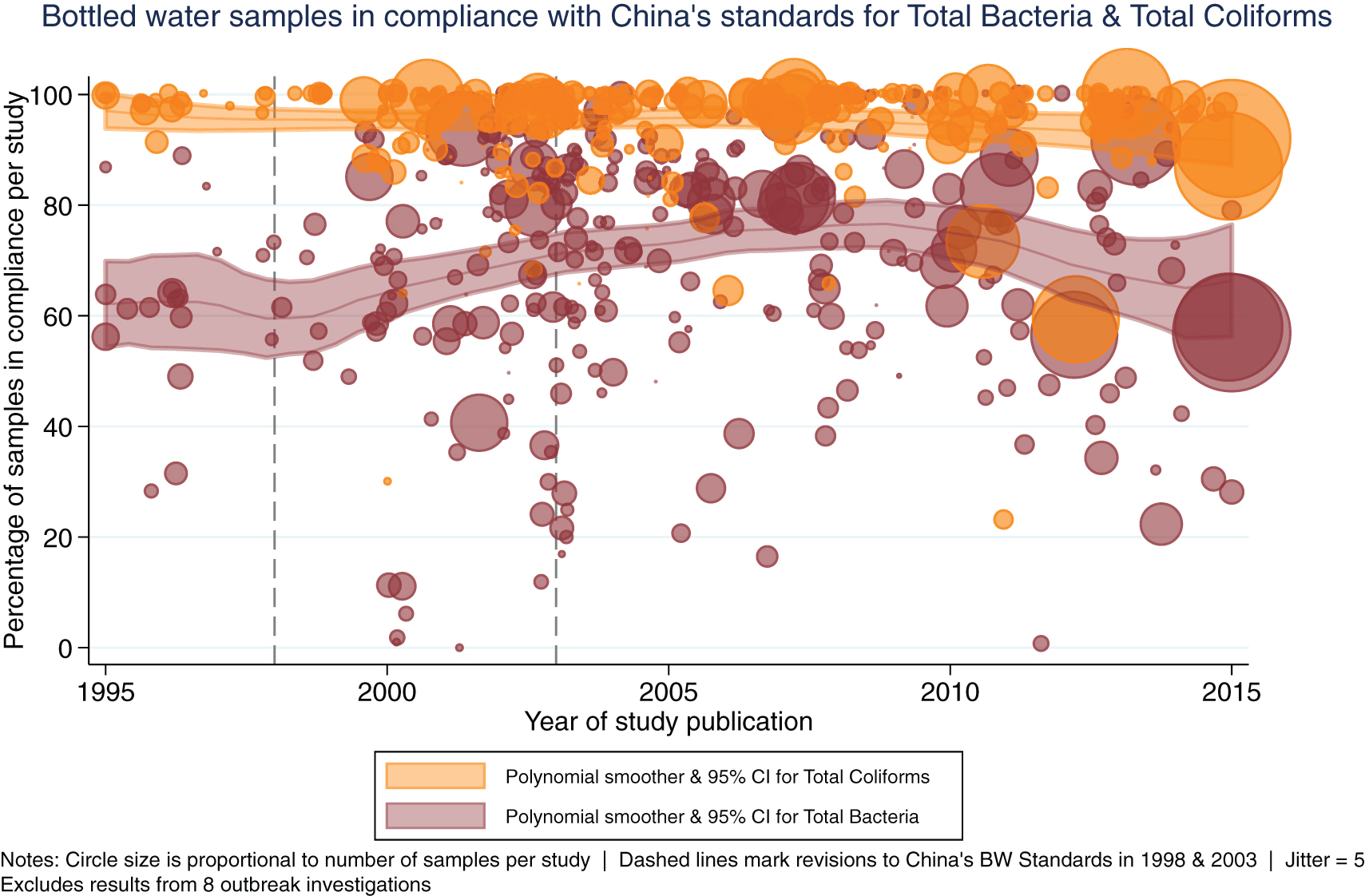
Bottled water quality and associated health outcomes: A systematic review and meta-analysis of 20 years of published data from China
Authors: Cohen, A., Cui, J., Song, Q., Xia, Q., Huang, J., Yan, X., Guo, Y., Sun, Y., Colford, J. M., & Ray, I.
Publication Year: 2022 | Journal / Publisher: Environmental Research Letters
Abstract/Summary: Bottled water is a rapidly growing yet relatively understudied source of drinking water globally. In addition to concerns about the safety of bottled water, the adverse environmental health and social impacts associated with bottled water production, distribution, consumption, and reliance are considerable. Our objective was to comprehensively review, analyze, and synthesize ∼20 years of publicly available data on bottled water quality and associated health outcomes in China. We conducted a systematic review and meta-analysis of publicly available studies of bottled water quality and associated health outcomes in China published between 1995 and early 2016 (in Chinese and English). We pre-specified and registered our study protocol, independently replicated key analyses, and followed standardized reporting guidelines. Our search identified 7059 potentially eligible records. Following screening, after full-text review of 476 publications, 216 (reporting results from 625 studies) met our eligibility criteria. Among many findings, 93.7% (SD = 10.1) of 24 585 samples tested for total coliforms (n = 241 studies), and 92.6% (SD = 12.7) of 7261 samples tested for nitrites (n = 85 studies), were in compliance with China’s relevant bottled water standards. Of the studies reporting concentration data for lead (n = 8), arsenic (n = 5), cadmium (n = 3), and mercury (n = 3), median concentrations were within China’s standards for all but one study of cadmium. Only nine publications reported health outcome data, eight of which were outbreak investigations. Overall, we observed evidence of stable or increasing trends in the proportions of samples in compliance over the ∼20 year period; after controlling for other variables via meta-regression, the association was significant for microbiological but not chemical outcomes (p = 0.017 and p = 0.115, respectively). Bottled water is typically marketed as being safe, yet in most countries it is less well-regulated than utility-supplied drinking water. Given the trend of increasing bottled water use in China and globally—and the associated environmental health impacts—we hope this work will help to inform policies and regulations for improving bottled water safety, while further highlighting the need for substantially expanding the provision of safe and affordable utility-supplied drinking water globally.
PDF on Publisher Website | PDF on OSF
Effects of boiling drinking water on diarrhea & pathogen-specific infections in low- & middle-income countries: A systematic review & meta-analysis
Authors: Cohen, A. & Colford, J. M.
Publication Year: 2017 | Journal / Publisher: American Journal of Tropical Medicine & Hygiene
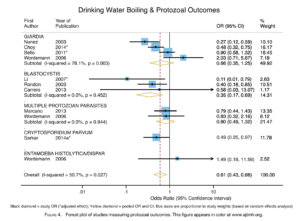 Abstract/Summary: Globally, approximately 2 billion people lack microbiologically safe drinking water. Boiling is the most prevalent household water treatment method, yet evidence of its health impact is limited. To conduct this systematic review, we searched four online databases with no limitations on language or publication date. Studies were eligible if health outcomes were measured for participants who reported consuming boiled and untreated water. We used reported and calculated odds ratios (ORs) and random-effects meta-analysis to estimate pathogen-specific and pooled effects by organism group and nonspecific diarrhea. Heterogeneity and publication bias were assessed using I2, meta-regression, and funnel plots; study quality was also assessed. Of the 1,998 records identified, 27 met inclusion criteria and reported extractable data. We found evidence of a significant protective effect of boiling for Vibrio cholerae infections (OR = 0.31, 95% confidence interval [CI] = 0.13–0.79, N = 4 studies), Blastocystis (OR = 0.35, 95% CI = 0.17–0.69, N = 3), protozoal infections overall (pooled OR = 0.61, 95% CI = 0.43–0.86, N = 11), viral infections overall (pooled OR = 0.83, 95% CI =0.7–0.98, N = 4), and nonspecific diarrheal outcomes (OR = 0.58, 95% CI = 0.45–0.77, N = 7). We found no evidence of a protective effect for helminthic infections. Although our study was limited by the use of self-reported boiling and non-experimental designs, the evidence suggests that boiling provides measurable health benefits for pathogens whose transmission routes are primarily water based. Consequently, we believe a randomized controlled trial of boiling adherence and health outcomes is needed.
Abstract/Summary: Globally, approximately 2 billion people lack microbiologically safe drinking water. Boiling is the most prevalent household water treatment method, yet evidence of its health impact is limited. To conduct this systematic review, we searched four online databases with no limitations on language or publication date. Studies were eligible if health outcomes were measured for participants who reported consuming boiled and untreated water. We used reported and calculated odds ratios (ORs) and random-effects meta-analysis to estimate pathogen-specific and pooled effects by organism group and nonspecific diarrhea. Heterogeneity and publication bias were assessed using I2, meta-regression, and funnel plots; study quality was also assessed. Of the 1,998 records identified, 27 met inclusion criteria and reported extractable data. We found evidence of a significant protective effect of boiling for Vibrio cholerae infections (OR = 0.31, 95% confidence interval [CI] = 0.13–0.79, N = 4 studies), Blastocystis (OR = 0.35, 95% CI = 0.17–0.69, N = 3), protozoal infections overall (pooled OR = 0.61, 95% CI = 0.43–0.86, N = 11), viral infections overall (pooled OR = 0.83, 95% CI =0.7–0.98, N = 4), and nonspecific diarrheal outcomes (OR = 0.58, 95% CI = 0.45–0.77, N = 7). We found no evidence of a protective effect for helminthic infections. Although our study was limited by the use of self-reported boiling and non-experimental designs, the evidence suggests that boiling provides measurable health benefits for pathogens whose transmission routes are primarily water based. Consequently, we believe a randomized controlled trial of boiling adherence and health outcomes is needed.
PDF on Publisher Website | PDF on OSF